Q. A 2004 ARVO report showed methicillin-resistant Staphylococcus aureus (MRSA) isolates to be resistant to fourth-generation fluoroquinolones. How serious is the potential for emerging resistance, given that the data reflected in-vitro testing?

A. After 95 MRSA ocular isolatescorneal ulcer or endophthalmitis caseswere tested for in-vitro susceptibility to fourth-generation and older fluoroquinolones, resistance rates were 74% for moxifloxacin, 77% for gatifloxacin, 91% for ciprofloxacin and 91% for ofloxacin.1
Arthur B. Epstein, O.D., of Ros-lyn Heights, N.Y., says that while the findings are disconcerting, they are not of immediate concern for most doctors because in-vitro testing and clinical performance do not necessarily equate. The immune system plays an important role in infection management and works in concert with antibiotics to clear surviving organisms, he says. Dr. Epstein adds that the extremely high levels that fourth-generation fluoroquinolones reach in corneal tissue are enough to overcome intermediate resistance.
Jay S. Pepose, M.D., Ph.D., of St. Louis, says in-vivo correlation is required to asses the seriousness of these findings. Its possible that the concentration of the drug at the corneal level may be much higher than what the researchers were testing, he says. A pharmacodyna-mic index relating corneal drug levels to the Minimum Inhibitory Concentration (MIC) of the keratitis isolates may show better clinical correlation. Still, he says that until there are enough patients on fluoroquinolones who do not respond, no firm conclusions can be reached.
James V. Aquavella, M.D., of Rochester, N.Y., says that while the bodys immune system has an effect, many in the general population have reduced immunity due to age and medication. He also says that although there are fixed amounts of medication in the in-vitro system, the bodys amounts will not be as fixed because, the patient may be missing their eye when instilling the drop, or there may be compliance issues.
Q. How do the findings of this report translate to the real world for clinical relevance?
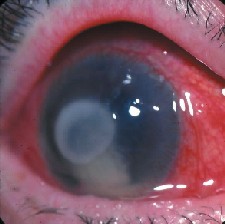
Will corneal ulcers, due to MRSA, become resistant to fourth-generation fluoroquinolones?
A. Dr. Epstein says the study is clinically relevant for patients who have corneal ulcers or other infections that do not respond to fourth-generation fluoroquinolones because MRSA may be the culprit. If youre in a tertiary setting, where MRSA infections are more common, I think the management paradigm is probably going to shift, he says.
Dr. Pepose says that while true clinical resistance to these drugs could eventually limit treatment options, for now, the following patients can benefit from this study: those who work in or are extensively exposed to hospital environments, are on long-term antibiotics or steroids and are scheduled for ocular surgery. Hospitals are great places to get MRSAs, so these folks should probably be prophylactically treated, he says. He adds that contact lens patients who work in hospitals and develop a red eye, should immediately remove their lenses, and see an eye doctor.
Dr. Aquavella believes that eye doctors should be vigilant in obtaining cultures and should not be as quick to prescribe the latest generation of fluoroquinolones for conjunctivitis, blepharitis or other superficial lesions. We should realize we may be contributing to the severity of the problem by not using a broad-spectrum, low-level antibiotic for these self-limiting kinds of infections, he says.
Others, however, believe the chance of developing resistance to various organisms is greatly reduced because fourth-generation fluoroquinolones require two sep-arate simultaneous mutations for resistance to occur.
1. Shah MK, Miller D, Ritterbrand D, et al. In-vitro resistant rates for fluoroquinolone antibiotics against methicillin resistant staphylococcus aureus (MRSA) ocular isolates from different geographic locations. ARVO Abstract #4924, 2004.

