 A 36-year-old Haitian female presented with symptoms of distortion and blurred vision in her left eye that have persisted for several years. She was born in
A 36-year-old Haitian female presented with symptoms of distortion and blurred vision in her left eye that have persisted for several years. She was born in
Her best-corrected visual acuity measured 20/20 O.D. and 20/30 O.S. Confrontation visual fields were full to careful finger counting O.U. Pupils were equally round and reactive, and she had no afferent pupillary defect.
Amsler grid testing was normal O.D., but showed a small area of central distortion O.S. Ocular motility testing was normal O.U. The anterior segment examination was unremarkable O.U. Her intraocular pressure measured 16mm Hg O.U.
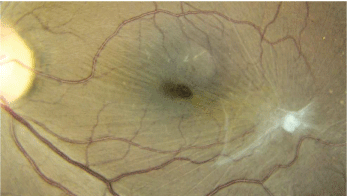
1. Our patients left eye exhibits a peculiar white lesion and macular changes.
Dilated fundus exam revealed a clear vitreous and moderate-sized cups, with good rim coloration and perfusion O.U. Examination of the right eye was completely normal, but the left eye showed changes in the macula and posterior pole, as seen in the fundus photograph (figure 1). We also obtained a spectral-domain optical coherence tomography (OCT) of the patients left eye (figure 2).
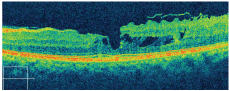
2. OCT of the patients macula O.S. What do you see?
Take the Retina Quiz
1. Based on the fundus photograph, how would you classify the changes seen in the left macula?
a. Epiretinal membrane with a pseudohole.
b. Epiretinal membrane with a lamellar hole.
c. Epiretinal membrane with a full-thickness hole.
d. Choroidal folds with a pseudohole.
2. How would you interpret the foveal changes seen on OCT?
a. Lamellar hole.
b. Pseudohole.
c. Full-thickness hole.
d. Cystoid macular edema (CME).
3. What does the white lesion seen in the fundus photo represent?
a. Persistent fetal scarring.
b. Fungal snowball.
c. Retinal granuloma.
d. Fibrous scar tissue.
4. What is the likely etiology?
a. Old toxoplasmosis infection.
b. Old Toxocara infection.
c. Retinal fibrosis from pars planitis.
d. Nonspecific fibrous scar tissue.
5. How should this patient be managed?
a. Pars plana vitrectomy and membrane peel.
b. Macular hole surgery.
c. Intravitreal injection of Avastin (bevacizumab, Genentech).
d. Observation.
For answers, see below.
Discussion
The clinical photos clearly show an epiretinal membrane in our patients macula O.S. The retinal striae are easily visible around the macula and emanate from the round, white lesion seen inferotemporal to the macula. The lesion represents a focal area of fibrous scar tissue. On clinical examination, the lesion was elevated and appeared to be superficial within the retina.
Based on the clinical appearance, the white lesion likely represents a granuloma. A granuloma is a small area of inflammation within a tissue that often develops as a result of injury or infection. Within the retina, it is unusual to see granulomatous lesions secondary to trauma; this granuloma was likely caused by an inflammatory event.
Because there is no vitreous inflammation, the granuloma appears inactive. At this point, it may be impossible to know exactly what caused the granuloma; however, it likely represents an old Toxocara infection.
Within the eye, Toxocara can have several distinct presentationsall of which yield a granulomatous inflammatory response.1 A posterior pole granuloma involving the macula will develop if the worm enters the eye via the short posterior ciliary arteries.
However, if the worm enters via the central retinal artery, patients may develop a peripheral granuloma. During the acute infection, patients may experience severe vitreous inflammation, which can lead to a retinal detachment.1
Our patients lesion is rather small compared to some Toxocara-induced granulomas. The invading organism may have been less virulent than normal, or her immune system was able to combat the organism without suffering severe scarring and inflammation. Our patient is lucky, but she is not completely out of the woods.
Our patient has a peculiar red lesion in her fovea O.S. that resembles a macular hole. In the presence of an epiretinal membrane, the majority of these lesions are typically pseudoholes.
A pseudohole is nothing more than a hole within an epiretinal membrane at the fovea, although it may resemble a full-thickness hole. It can be difficult to differentiate between pseudoholes and full-thickness holes, but there are some distinguishable features to look for. Specifically:
Full-thickness holes usually demonstrate a complete loss of the
photoreceptor elements, while pseudoholes feature a normal foveal depression, often with obvious steepening of the walls.2
Full-thickness holes have an encompassing cuff of fluid and typically appear completely round. In contrast, psuedoholes do not have the surrounding cuff of fluid and usually appear oval or elliptical.
Patients with pseudoholes often demonstrate somewhat decent visual acuity (sometimes up to 20/20), whereas patients with full-thickness holes tend to see 20/100 or worse.2
Our patients red lesion appears to be a full-thickness hole; however, the inner and outer photoreceptor elements are still present. We diagnosed her with a lamellar, or partial-thickness, hole.
J. Donald M. Gass, M.D., first described lamellar macular holes in 1975, when he identified a macular lesion that resulted from CME.3 Since then, the term lamellar hole has been used to describe the abortive process for patients who are developing a full-thickness macular hole. Understandably, these lesions are quite rare and are almost never seen. However, with OCT we are now able to visualize the retinal anatomy with near microscopic resolution. Now, these rarely-seen macular lesions are being diagnosed more frequently and accurately.
In a recent study of 19 eyes with lamellar macular holes, only seven eyes were properly diagnosed on clinical examination, whereas spectral domain OCT accurately diagnosed 17 eyes.4 Interestingly, the lamellar holes shared several common features on OCT, including:
An irregular foveal contour.
A break in the inner fovea.
Separation of the inner and outer foveal layers, resulting in an intraretinal split.
Absence of a full-thickness defect with intact photoreceptors posterior to the area of foveal dehiscence.4
Our patient exhibited all the aforementioned features. Because she had good visual acuity (20/30 O.S.), we initially elected to observe her in six weeks, then in three months and then twice a year.
We believe that her lamellar hole will not progress. Also, we obtained blood studies to try to identify the cause of the granulomatous lesion; but, everything came back negative, including Toxocara titres.
Retina Quiz Answers: 1) a; 2) a; 3) c; 4) b; 5) d
1. Wilkinson CP. Ocular Toxocariasis. In: Ryan SJ. Schachat AP, Murphy RP, (eds). Retina, vol. 2. Medical Retina, 3rd ed.
2. Gass J, Donald M. Stereoscopic Atlas of Macular Diseases: Diagnosis and Treatment, vol. 2.
3. Gass JD. Lamellar macular holes: a complication of cystoid macular edema after cataract extraction: a clinicopathlogic case report. Trans Am Ophthalmol Soc 1975;73:231-50.
4. Witkin AJ, Ko TH, Fujimoto JG, et al. Redefining lamellar holes and the vitreomacular interface: an ultrahigh resolution optical coherence tomography study. Ophthalmogy 2006 Mar;113(3):388-97.

