Blepharitis is a prevalent disorder with many recognized therapeutic options. Hygienic regimens, topical agents and even oral medications are used in management. But, how many of us truly understand the role of each therapeutic measure, or use them appropriately and effectively? Many prac- titioners have pre-printed education sheets for blepharitis, that describe the process of lid soaks and/or lid scrubs in detail. Unfortunately, simply distributing literature to patients does not ensure appropriate management. More importantly, not every case of blepharitis responds favorably to simple lid hygiene. Successful therapy must be tailored to each individual patient.
Lid hygienein the form of warm compresses and lid scrubsplays an important role in the initial management of infectious blepharitis (Staph. blepharitis). Heat, combined with the application of a mild detergent, helps remove the debris that serves as a potential substrate for bacterial colonization, and diminishes excessive bacteria and their exotoxins.
Still, the application of a good, broad-spectrum antibiotic ointment is probably more effective in alleviating the acute symptomatology of this disorder. Many practitioners have favored erythromycin for this purpose. However, macrolide anti- biotics are merely bacteristatic (rather than bactericidal), and their pharmacokinetics rely upon a time-dependent rather than dose-depend- ent mechanism. So, a much better option for infectious blepharitis would be an aminoglycoside (e.g., tobramycin) or a fluoroquinolone (e.g., ciprofloxacin) applied twice daily.
|
|
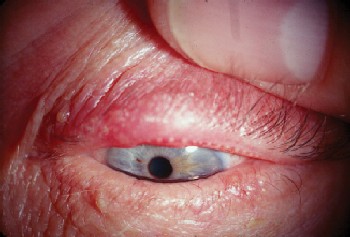
| There can be advanced cases of blepharitis, as seen above with this patent who has meibomian gland disease secondary to rosacea. |
Oral antibiotics are rarely necessary in infectious blepharitis, as bacterial colonization occurs superficially on the lids. Topical agents are actually more efficacious than systemic medications in these cases. In cases of significant eyelid inflammation, a combination antibiotic-corticosteroid ointment, such as TobraDex (tobramycin and dexamethasone, Alcon), likely offers the best therapy.
Seborrheic Blepharitis
Seborrhea represents an inflammatory dermatologic condition and does not result from an infectious process. Warm compresses applied b.i.d. to q.i.d. help melt away the waxy scales associated with seborrhea. Likewise, lid scrubs using a very dilute detergent-based solution (e.g., Johnsons Baby Shampoo or Neutrogena soap) can help remove the excess sebum. Commercially available eyelid cleansing pads may provide a more convenient, if more costly, means of achieving this outcome.1
Seborrhea has been associated with a pathogenic yeast (Pityrosporum ovale, also known as Malas-sezia furfur). Shampoos contain- ing antifungal agents, such as zinc pyrithione and selenium sulfide are available. However, these shampoos are not indicated for use in or around the eye. Topical steroid preparations are likewise discouraged. Although steroids may provide short-term relief, they tend to hasten recurrences and foster dependence. Moreover, the potential ocular risks associated with long-term topical steroid use are a significant deterrent.
Advise patients with associated seborrheic dermatitis to seek dermatologic consultation, as alleviating the underlying condition may further help with blepharitis management. In addition to special shampoos, topical ketoconazole 2% cream and oral itraconazole may treat more resistant cases. However, both have been studied in the treatment of seborrheic blepharitis with mixed results.2-4
Meibomian Gland Dysfunction (MGD)
MGD is a multifactorial disorder, but infection is not a major cause. While enhanced bacterial growth is associated with MGD, it is a secondary phenomenon that occurs deep within the glands, outside the reach of most topical agents. Some practitioners still recommend topical antibiosis for MGD, but in our experience, this is not terribly efficacious. Lid hygiene plays a much more significant role in the initial and ongoing management. Warm compresses combined with vigorous lid massage soften the thickened secretions within the meibomian ducts and stimulate normal sebaceous flow from these glands.
Lid scrubs, though, are not as useful. One study showed that MGD actually results in saponificationthat is, the creation of detergentwithin the tear film, due to the enhanced formation of free fatty acids and inflammation.5 The addition of more detergent to an already unstable ocular surface only compromises the tear film further and may contribute to poor patient compliance.1,5 Therefore, it is probably best to refrain from lid scrub therapy when managing MGD.
Oral tetracycline and its derivatives (e.g., doxycycline and minocycline) are important to consider in more recalcitrant cases. Tetracycline appears to inhibit bacterial lipase production and reduce free fatty acids, which accounts for its great efficacy in MGD management. This is particularly true for those patients who have ocular rosacea.6 In addition, a recent study showed that tetracyclines have anti-inflammatory properties and specifically inhibit matrix metalloproteinase-9 and interleukin-1, both powerful modulators of inflammation.7 While we may not fully comprehend how these drugs work, a regimen of oral doxycycline 100mg b.i.d. x 4 weeks, then q.d. x 4-8 weeks, is often very effective in MGD management.8
Another potential treatment option for MGD is the nutraceutical route. Proponents of this ther- apy maintain that meibomian secretions are derived from omega-3 essential fatty acids, which can only be obtained through dietary intake. A recent report suggests that flax- seed oil may help to produce clearer and thinner meibomian secretions in patients who have evaporative dry eye.9 Other studies have shown that systemic administration of essential fatty acids diminishes the inflammation and symptomology associated with MGD and dry eye.10 More prospective clinical trials are necessary to determine if nutraceuticals represent a legitimate treatment option for MGD, but the anecdotal evidence is compelling.
Finally, Restasis (cyclosporine, Allergan) may also have a beneficial effect in patients who have MGD. A recent report suggests that topical cyclosporine diminishes meibomian gland inclusions and reduces lid margin injection in patients who have posterior blepharitis.11,12 Other long-term controlled studies have yet to corroborate these reports, but this may prove to be an added advantage for those dry eye syndrome patients who use Restasis.
While there are numerous beneficial therapies for blepharitis, practitioners must remain wary of adop- ting a one-size-fits-all attitude in the management of this disorder. Clearly, not all these modalities are suitable for every patient, and some therapeutic choices may actually worsen the condition if applied haphazardly.
The key to management is careful differentiation, appropriate and conservative initial therapy, and vigilant follow-up to determine if the treatment is effective. n
- Key JE. A comparative study of eyelid cleaning regimens in chronic blepharitis. CLAO J 1996 Jul; 22:209-12.
- Baysal V, Yildirim M, Ozcanli C, Ceyhan AM. Itraconazole in the treatment of seborrheic dermatitis: a new treatment modality. Int J Dermatol 2004 Jan; 43(1):63-6.
- Nelson ME, Midgley G, Blatchford NR. Ketoconazole in the treatment of blepharitis. Eye 1990; 4 (Pt 1):151-9.
- Ninomiya J, Nakabayashi A, Higuchi R, Takiuchi I. A case of seborrheic blepharitis; treatment with itraconazole. Nippon Ishinkin Gakkai Zasshi 2002; 43(3):189-91.
- Romero JM, Biser SA, Perry HD, et al. Conservative treatment of meibomian gland dysfunction. Eye Contact Lens 2004 Jan; 30(1):14-9.
- Dougherty JM, McCulley JP, Silvany RE, Meyer DR. The role of tetracycline in chronic blepharitis. Inhibition of lipase production in staphylococci. Invest Ophthalmol Vis Sci 1991; 32(11):2970-5.
- Solomon A, Rosenblatt M, Li DQ, et al. Doxycycline inhibition of interleukin-1 in the corneal epithelium. Invest Ophthalmol Vis Sci 2000; 41(9):2544-57.
- Quarterman MJ, Johnson DW, Abele DC, et al. Ocular rosacea. Signs, symptoms, and tear studies before and after treatment with doxycycline. Arch Dermatology 1997 Jan; 133(1):49-54.
- Kronemyer B. Dry eye successfully treated with oral flaxseed oil. Oc Surg News 2000; 10(11):147-8.
- Barabino S, Rolando M, Camicione P, et al. Systemic linoleic and gamma-linolenic acid therapy in dry eye syndrome with an inflammatory component. Cornea 2003 Mar; 22(2):97-101.
- Perry HD, Donnenfeld ED. Dry eye diagnosis and management in 2004.Curr Opin Ophthalmol 2004 Aug; 15(4):299-304.
- Perry HD, Doshi S, Donnenfeld ED, et al. Double masked randomized controlled study evaluating topical 0.05% cyclosporine A in the treatment of meibomian gland dysfunction (posterior blepharitis). Invest Ophthalmolol Vis Sci 2003; 44: E-abstract 1395.