 History
History
A 70-year-old black female presented with a chief complaint of blurred vision at near O.U. that has gradually worsened during the previous four months.
Her systemic history was remarkable for longstanding hypertension, which is medically controlled by her physician. She denied any allergies to medications or other substances.
Diagnostic Data
Her best-corrected visual acuity was 20/25 O.U. at distance and near. External examination was normal, with no evidence of afferent pupillary defect O.U. The patients intraocular pressure measured 15mm Hg O.U. Dilated fundus examination was unremarkable O.U. Anterior segment structures were normal O.S.
The significant anterior segment finding O.D. is illustrated in the photograph.
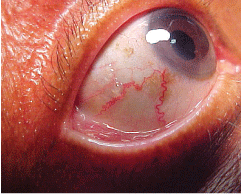
The right eye of a 70-year-old female who presented with a chief complaint of blurred vision in both eyes at near.
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? Whats the likely prognosis?
Discussion
The diagnosis in this case is low flow, dural venous sinus fistula. Additional testing for this case included magnetic resonance imaging (MRI) with and without gadolinium. The fistula thrombosed after MRI with gadolinium.
If MRI is contraindicated, order computed tomography (CT) scans using very thin axial and coronal sections, with and without contrast. Consider the use of magnetic resonance angiogram (MRA) and/or conventional angiography. A cerebrospinal fluid examination may be helpful, but is rarely used.1
If you suspect an inflammatory or infectious etiopathology, order the following bloodwork: angiotensin-converting enzyme, Lyme titer, rapid plasma reagin and/or fluorescent treponemal antibody absorption.2
Management of patients with cavernous sinus and superior orbital fissure lesions depend on the patients age, acuteness of presentation, speed of progression, presence of pain, history of systemic disease or tumors, and presence of accompanying features (i.e. cranial nerve III, IV and VI palsy; resultant diplopia; or corneal involvement secondary to the worsening exophthlmos). Patients with more subtle fistulas are often diagnosed with conjunctivitis.1-4
Immediately evaluate patients who present with fever, somnolence or a toxic appearance for evidence of cavernous sinus thrombosis or mucormycosis. Patients who present with prominent arterialization of conjunctival vessels, proptosis and bruits must be evaluated for direct carotid cavernous fistula.1
Use arteriography to diagnose direct or indirect carotid-cavernous fistula.1 However, both MRI and MRA may demonstrate enlargement of the superior ophthalmic vein or the actual fistula.1,3 Other helpful procedures include Doppler ultrasound, color Doppler, and measurement of ocular pulse amplitude. Reversal of flow may be demonstrated in the superior ophthalmic vein.1,3,4
Direct, internal carotid artery-to-cavernous sinus fistulas should be treated with balloon occlusion of the connection between the carotid artery and cavernous sinus by an interventional neuroradiologist. Neurosurgery, which involves occlusion of the carotid artery both above and below the site of the fistula, may be required.4
If there is no threat to vision, simply follow asymptomatic dural arteriovenous fistulas.1,3,4 More than 50% of patients with this type of fistula experience spontaneous thrombosis, with resolution after angiography. On some occasions, spontaneous thrombosis may be associated with retinal vein occlusions and vision loss. In cases that involve a threat to vision, an interventional radiologist should perform selective arteriography with occlusion of the feeder vessels.1
1. Moster M. Paresis of Isolated and Multiple Cranial Nerves and Painful Ophthalmoplegia. In: Yanoff M, Duker JS (eds). Ophthalmology.
2. Bhatti MT. Orbital syndromes. Semin Neurol 2007 Jul;27(3):269-87.
3. Eddleman CS, Surdell D, Miller J, et al. Endovascular management of a ruptured cavernous carotid artery aneurysm associated with a carotid cavernous fistula with an intracranial self-expanding microstent and hydrogel-coated coil embolization: case report and review of the literature. Surg Neurol 2007 Nov;68(5):562-7.
4. Miller NR. Diagnosis and management of dural carotid-cavernous sinus fistulas. Neurosurg Focus 2007;23(5):E13.

