A 58-year-old white female presents for an examination complaining of unusual and excess tearing O.U. that has been occurring sporadically for the past several months, but has gotten worse over the past several weeks. It seems more severe in her right eye than her left.
A 58-year-old white female presents for an examination complaining of unusual and excess tearing O.U. that has been occurring sporadically for the past several months, but has gotten worse over the past several weeks. It seems more severe in her right eye than her left.
She reports that occasionally the tears run down her cheeks. She denies dryness, pain, visual change or irritation. In fact, other than her constantly weepy eyes, she demonstrates perfect ocular health.
Upon gross inspection, there is some mild wetness of each eye. However, it is so subtle that it would have been overlooked or dismissed, save her complaints. While seemingly insignificant, this constant tearing is clearly making the patient unhappy. This month, we attempt to provide an algorithm of clinical thinking to follow when patients present with chronic epiphora.
Ectropion often leads to chronic epiphora.
Epiphora Defined
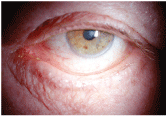
Epiphora is the spillover of tears from the eye onto the lids and ocular adnexa. It is not a diagnosis, but a clinical finding that suggests ocular abnormality. Determining the underlying cause can be challenging; numerous conditions can cause it.1-5
Acute epiphora tends to be more easily diagnosable and attributable to an underlying cause than chronic epiphora. In acute cases, foreign bodies, trichiasis or new onset allergic reactions provoke the patient to seek immediate care, and the cause is often easily discernible. In contradistinction, chronic epiphora has been present for a long period of time in a clinically smoldering manner, and the cause may not be as apparent in such cases.
Acute epiphora usually resolves following removal of the irritant. Chronic epiphora, however, often does not resolve, as the cause is not identified or removed. Symptoms may be exacerbated by environmental factors, such as wind, pollen counts and pollution, as well as fatigue, strain or emotional stress.
Examining Epiphoras Causes
Environment and precipitating factors. Taking a thorough history is paramount in determining the cause of epiphora, and the first step is verifying whether the epiphora is acute or chronic. If it is acute, determine the onset and precipitating factors. Due to the short-term nature of the condition, this is usually easily accomplished.
Find any associated signs or symptoms. Patients who complain of itchiness and rub their eyes are likely suffering from allergies, and excess tearing is the eyes attempt to flush away the offending antigens.
Identify the environment most likely to precipitate the tearing. Epiphora that is worse outdoors than indoors is likely due to pollen, pollution or other allergens assaulting the eye. If there is a seasonal component, allergies are the likely cause, and antihistamines may be the best treatment. If the tearing is worse indoors, air-conditioning, fans or dry forced-air heat may precipitate tear evaporation and subsequent dry eye.
Determine if the patient has any grittiness or dryness. Patients with dry eye often suffer from reflex tearing, which is the eyes attempt to compensate for poor tear quality or inadequate surface wetting. Inspect the corneal surface for punctate epithelial disruption or rapid tear film break-up time (TFBUT), two classic manifestations of dry eye. Look for signs of meibomian gland disease, which can contribute to dry eye and ocular surface disease.
Ask the patient if eye rubbing improves or worsens the feeling. Patients who feel worse typically suffer from allergies, while those who feel better with increased tearing after eye rubbing are suffering from dry eye and/or blepharitis. Managing the patients ocular allergies or dry eye likely will decrease the epiphora.
Proper lacrimal drainage. Inspect the eyes for proper lid-globe congruity. Make sure that the eyelid smoothly apposes the globe. If there is entropion or trichiasis, the rubbing of the lashes against the cornea and conjunctiva becomes an irritant that stimulates excess tear production, a common cause of acute epiphora.
A more likely cause for chronic epiphora, however, is ectropion. When the eyelid does not appose the globe properly, the punctal drainage system will not function properly. Tears pool in the conjunctival sulcus until they spill over the eyelid, rather than drain through the canalicular system. Even if the lower lid seems to be in normal apposition with the globe, gently pull it away from the globe. Normally, it should snap back. In elderly patients and those with loose skin, there will be a period of acquired ectropionthe eyelid does not immediately reappose the globe, and tear drainage is impeded. These patients may need lid-tightening surgery to properly reposition the lid to the globe.
The lower eyelid puncta should not be visible unless the eyelid is manually everted. If the lower punctum is visible without manually everting or touching the eyelid in any way, this may be the problem. If the punctum does not appose the globe, tears cannot be properly draineda subtle form of ectropion. Also, look to see that the puncta are not stenosed. If they appear closed, gentle dilation with a punctal dilator may solve the problem.
Obstruction may also occur in the canalicular system, such as in canalicular stenosis or canaliculitis, dacryocystitis, or lacrimal sac tumors. Conjunctivochalasis, a condition in which redundant, sagging conjunctiva covers the lacrimal punctum and impedes drainage through the nasolacrimal canaliculus, may also be observed on biomicroscopy.6,7
Punctal or canalicular dilation and irrigation is the most common management for stenosis of the lacrimal system. In many cases, the procedure is both diagnostic and therapeutic. In these cases, the procedure identified the problem as a blockage of the nasolacrimal drainage system and effectively eliminated the blockage at the same time.
However, blockage of the nasolacrimal system is not the cause in a significant number of cases of epiphora. We very rarely perform this procedure and have found that successfully relieving epiphora through dilation and irrigation is the exception rather than the rule. Additionally, vigorous flushing of saline through the nasolacrimal drainage system or inappropriate placement of the dilator or probe can damage this system very easily. So, dilation and irrigation should not be done commonly or cavalierly. Additionally, in acute cases of epiphora where canalicular infection is suspected, dilation and irrigation is contraindicated, as it can cause rupture and infection spread.
In cases of chronically flaccid or stenotic puncta, laser punctoplasty or ampullotomy can enlarge the outflow orifice.8,9 If the blockade exists more distally within the nasolacrimal system, probing alone may be inadequate to alleviate the problem. In such cases, dacryocystorhinostomy (DCR) creates a surgical bypass of the common canaliculus directly into the nasal mucosa.
Neurogenic causes. Corneal exposure secondary to proptosis (from a retro-orbital mass) or facial nerve palsy may induce reflex tear production. Epiphora may be encountered with compressive irritation of the nervus intermedius fibers.10 In a chronic case of epiphora unresponsive to conventional therapy, suspect a neurogenic hypersecretory disorder. Refer the patient to a neurologist.
After extensive history and examination, no overt cause explained our patients epiphora. She couldnt tell if it worsened indoors or outdoors, and she could give no history of exposure to direct wind, air conditioning, or heat. Her ocular surface and TFBUT were normal. There was excellent lid-globe congruity and the puncta were wide open.
Upon discussing her history, she did acknowledge some mild itching O.U., but this symptom paled next to the epiphora, in her opinion. Nevertheless, we prescribed a topical antihistamineboth to remove any possible allergic component to her condition and to take advantage of the antimuscarinic effect of the antihistamine and dry her out.
One month later, she reported that she felt better and was not nearly as bothered by epiphora. Did the antihistamine dry her out or actually combat an allergen? Or, did the drop soothe a subclinical dry eye? Regardless, the therapy seemed to solve her problem.
1. Narayanan K, Barnes EA. Epiphora with eyelid laxity. Orbit 2005 Sep;24(3):201-3.
2. Singh Bhinder G, Singh Bhinder H. Reflex epiphora in patients with dry eye symptoms: role of variable time Schirmer-1 test. Eur J Ophthalmol 2005 Jul-Aug;15(4):429-33.
3. Tu AH, Chang EL. Botulinum toxin for palliative treatment of epiphora in a patient with canalicular obstruction. Ophthalmology 2005 Aug;112(8):1469-71.
4. Berdy GJ, Hedqvist B. Ocular allergic disorders and dry eye disease: associations, diagnostic dilemmas, and management. Acta Ophthalmol Scand Suppl 2000;(230):32-7.
5. Bielory L. Ocular allergy and dry eye syndrome. Curr Opin Allergy Clin Immunol 2004 Oct;4(5):421-4.
6. Liu D. Conjunctivochalasis. A cause of tearing and its management. Ophthal Plast Reconstr Surg 1986;2(1):25-8.
7. Georgiadis NS, Terzidou CD. Epiphora caused by conjunctivochalasis: treatment with transplantation of preserved human amniotic membrane. Cornea 2001 Aug;20(6):619-21.
8. Kashkouli MB, Beigi B, Astbury N. Acquired external punctal stenosis: surgical management and long-term follow-up. Orbit 2005 Jun;24(2):73-8.
9. Awan KJ. Laser punctoplasty for the treatment of punctal stenosis. Am J Ophthalmol. 1985 Aug;100(2):341-2.
10. Keegan DJ, Geerling G, Lee JP, et al. Botulinum toxin treatment for hyperlacrimation secondary to aberrant regenerated seventh nerve palsy or salivary gland transplantation. Br J Ophthalmol 2002 Jan;86(1):43-6.