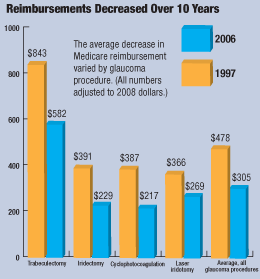
 Medicare reimbursement for glaucoma surgeries has decreased by an average of 36% in the last 10 years, reports a study in the July Archives of Ophthalmology. The study, which examined cases of trabeculoplasty, trabeculectomy, shunt instillation, iridectomy, iridotomy, iridoplasty and cyclophotocoagulation, also found that the quantity of each procedure per year did not seem to affect its reimbursement.
Medicare reimbursement for glaucoma surgeries has decreased by an average of 36% in the last 10 years, reports a study in the July Archives of Ophthalmology. The study, which examined cases of trabeculoplasty, trabeculectomy, shunt instillation, iridectomy, iridotomy, iridoplasty and cyclophotocoagulation, also found that the quantity of each procedure per year did not seem to affect its reimbursement.
Using a random sample of elderly Medicare beneficiaries not enrolled in an HMO, researchers determined that there was a decrease in the total number of glaucoma surgeries from 1997 to 2001, which then reversed and increased through 2006. But, the total annual reimbursement payment for these procedures was at its highest, $161 million, in 1997. In 2001, the total annual payment was $110 million.
From 1997 to 2006, the average overall payment of all procedures fell by 36%. This decrease could not be attributed to the quantity of procedures. For instance, payment for trabeculectomy with no prior surgery decreased by 35%, but procedure quantity decreased by 55%, while cyclophotocoagulation payment dropped by 44%, but claims quadrupled.
"Medicare has limited funds and increasing amounts of people seeking care through it, so it has to cut payments to control the growth in cost," says optometrist Daryl Mann, of
The decline stems from Medicare's fixed budget. "During the past several years, the number of services billed for certain diagnoses--e.g., primary open-angle glaucoma--have risen dramatically," says Charles B. Brownlow, O.D., associate director of the AOA Third Party Center. "This is partially due to more cases being diagnosed and also due to new technologies used in the diagnosis and management of POAG, many of which involve very expensive instrumentation. Medicare only has so many dollars to spend each year, so it's understandable that the Medicare reimbursements per procedure will be decreased as the number of procedures increase."
Researchers found no evidence that surgeons took reimbursement into consideration when determining the best procedure for each patient. "We try to do whatever is the appropriate procedure done for the patient," Dr. Mann says.
But, the decline in reimbursement is something that practitioners must take into account in their practices. "Just considering the drop in conversion factor from 2008 to 2009 (5.7%), its clear that all providers have to feel the pinch," Dr. Brownlow says. "Some doctors consider government programs to be a kind of charity work, understanding that the plans are not meant to reimburse them at their usual charges. But even so, 5.7% is significant."
And, a system with fixed limits will not be able to hold the increasing amount of patients who depend on it for glaucoma treatment. "Glaucoma is a disease that increases in frequency with age," says Dr. Mann. "And, these procedures are going to increase in their frequency simply because we will have more patients with glaucoma, which will put more stress on the payment side of the health care system."
Schmier JK, Covert DW, Lau EC, Robin AL. Trends in annual Medicare expenditures for glaucoma surgical procedures from 1997 to 2006. Arch Ophthalmol. 2009 Jul;127(7):900-5.

