A 51-year-old white female presented with distortion and blurred vision in her left eye that had persisted for a month. Since childhood, she has had a long history of eye problems. She began wearing glasses for myopia correction in kindergarten. The myopia continued to progress during her teenage years; however, she always enjoyed excellent vision in both eyes with optical correction.
A 51-year-old white female presented with distortion and blurred vision in her left eye that had persisted for a month. Since childhood, she has had a long history of eye problems. She began wearing glasses for myopia correction in kindergarten. The myopia continued to progress during her teenage years; however, she always enjoyed excellent vision in both eyes with optical correction.
Then, in her early 20s, our patient began experiencing retinal problems that required multiple laser treatments in both eyes. The laser correction negatively affected the central visual acuity in her right eye, prohibiting clear vision. Thankfully, however, her left eye achieved a better outcome (20/20). But recently, our patient began noticing blurred vision and distortion O.S.
|
|
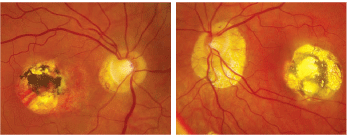
| 1,2. The posterior poles of our patients eyes show interesting macular lesions (O.D. left, O.S. right). What can you deduce? |
On examination, her best-corrected visual acuity measured 20/400 O.D. and 20/40 O.S. Confrontation visual fields were full to careful finger counting O.U. Pupils were equally round and reactive, with no afferent pupillary defect. Amsler grid testing showed a dense, central scotoma O.D. and a paracentral scotoma O.S., with central metamorphopsia. Ocular motility testing was normal. The anterior segment examination of both eyes was unremarkable. Her intraocular pressure measured 11mm Hg O.U.
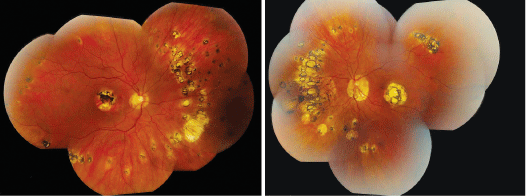 |
| 3, 4. The peripheral montage images (O.D. left, O.S. right) also show peripheral retinal lesions. What do these represent? |
Her dilated fundus exam revealed a clear vitreous O.U. Obvious fundus changes are apparent in both eyes (figures 1-4). Additionally, we ordered a fluorescein angiogram (figure 5) and a spectral domain optical coherence tomography of her left eye (figure 6).
|
|
|
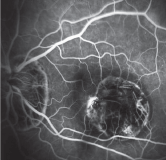
| 5. A mid-phase fluoresein angiogram of the left eye. What does it reveal? |
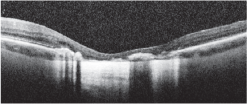
6. An SD-OCT slice through the macula in the left eye. |
Take the Retina Quiz
1. How do you account for the prominent macular scars in both eyes?
a. Myopic degeneration.
b. Chronic central serous chorioretinopathy with subsequent scarring.
c. Laser scars.
d. Old toxoplasmosis infection.
2. What does the FA show in the left eye?
a. Blockage.
b. Window defect at the edge of the scar.
c. Leaking at the edge of the scar secondary to choroidal neovascularization.
d. Nonspecific hyperfluorescence around the edges of the scar.
3. How do you explain the symptoms in the left eye?
a. Expansion of the macula scar.
b. Reactivation of toxoplasmosis
infection.
c. Recurrent CNV.
d. Serous detachment of her macula.
4. What is the likely diagnosis for this patient?
a. Degenerative myopia.
b. Toxoplasmosis infection.
c. Ocular histoplasmosis.
d. Multifocal choroiditis and panuveitis.
5. How should this patient be managed?
a. Observation.
b. Bactrim (sulfamethoxazole and trimethoprim, AR Scientific, Inc.).
c. Avastin (bevacizumab, Genentech) injection and observation.
d. Kenalog (triamcinolone, Bristol-Myers Squibb) injection and observation.
For answers, see below.
Discussion
Our patient has some very striking fundus changes in both eyes, and the most obvious are very prominent macular scars. The macular scar in the right eye involves the center of her fovea, which explains why she sees 20/400.
The macular scar in the left eye is just as large as the macular scar in the right, so it is surprising that she can see 20/40. Even more shocking, however, is that she saw 20/20 in this eye before presenting for this evaluation.
So, what is causing the problem in her left eye? On clinical examination of her macula, she manages to fixate just at the edge of the scar in an area where the macula appears to be spared. Unfortunately, there appears to be some retinal thickening and serous fluid. The FA shows an area of leakage with hyperfluoresence at the edge of the scar that involves her macula. The SD-OCT also shows an area of fluid that is consistent with what was seen on FA. Sadly, this presentation is very typical for CNV.
This is not the first time our patient has had this type of problem. Indeed, the macular scars, as well as her case history, provide evidence that she had prior episodes of CNV that resulted in multiple laser procedures more than 25 years ago. At that time, she was told that she had ocular histoplasmosis, which lead to CNV.
Histoplasmosis develops from exposure to the fungus Histoplasma capsulatum via the respiratory tract. The geographic areas endemic for this condition include the
Indeed, our patient has many features consistent with ocular histoplasmosis. In fact, her peripheral retinal changes are quite pronouncedalmost overly exaggerated for what is typically seen in patients with peripheral histo-spots.
Our patient demonstrates mid-peripheral circumferential, focal, atrophic scars in both eyes that seem to be denser in the nasal retinas. Some of the scars are even
confluent, which is unusual for histoplasmosis. It is also unusual to observe a symmetric pattern of histo-spots not only in, but also between both eyes.
Interestingly, our patient did not grow up in an area endemic for histoplasmosis. She was raised in a large city in
The bottom line: We are uncertain if our patient exhibits histoplasmosis or degenerative myopia. A definitive diagnosis is difficult because our patient's complications began more than 25 years ago. Who knows to what extent her retinas were involved back then? It would also be interesting to know when the peripheral retinal changes began and how they have progressed during the last 25 years. We may never know the answers to these questions. Regardless, we still have to treat the CNV in her only functioning eye.
Fortunately, with the advent of anti-vascular endothelial growth factor therapy, we now have a way to improve vision in patients with CNV. Our patient underwent four intravitreal Avastin injections during a six-month period. Her visual acuity improved to 20/30 O.S. following the first injection. After receiving four injections, she improved to 20/20.
We will continue to monitor her condition with both SD-OCT and FA.
Answers: 1) C; 2) C; 3) C; 4) C; 5) C.
1. Edwards LB, Acquaviva FA,
2. Hawkins BS, Alexander J, Solomon SD, et al. Ocular Histoplasmosis. In: Ryan SJ, Schachat AP, Murphy RP (eds). Retina, Vol. II: Medical Retina, 4th ed.