 Ocular tissues have a limited capacity for regeneration. As such, ocular inflammation can lead to severe vision loss. However, the eye has a special relationship with the immune system; it has the ability to quench unwanted immune-mediated inflammation. This is known as immune privilege.1
Ocular tissues have a limited capacity for regeneration. As such, ocular inflammation can lead to severe vision loss. However, the eye has a special relationship with the immune system; it has the ability to quench unwanted immune-mediated inflammation. This is known as immune privilege.1
An important part of immune privilege is anterior chamber-associated immune deviation (ACAID). ACAID is an immunoregulatory process that is initiated when an antigen enters the eye. ACAID suppresses the initiation of antigen-specific inflammation, culminating in the tight regulation of immune-mediated inflammation and the preservation of visual function.1
We do encounter situations in clinical practice when the eye’s immune privilege is overcome—for example, in cases of uveitis and ocular surface inflammatory disease. That’s when we step in with agents to suppress the immune response. Immunomodulation is an adjustment of the body’s immune response to a desired level, usually by agents that activate or suppress its function. For instance, the success of pharmacotherapy with steroids for uveitis is well documented. Clinical studies have also shown the benefit of topical immunomodulation for conditions such as dry eye, vernal keratoconjunctivitis and atopic blepharoconjunctivitis.2,3
Case Report
• History. A 48-year-old white female presented complaining of bilateral foreign body sensation, intermittent blur, burning and irritation. She could not wear her soft multifocal contact lenses for more than two to three hours per day. Her symptoms had started four years prior and progressively worsened. Her systemic history was remarkable for systemic lupus erythematosus, which was treated with hydoxychloroquine 200mg b.i.d. She recently began to experience hot flashes and irregular menstrual cycles. Her gynecologist did not recommend menopausal hormone therapy at that time.
• Diagnostic data. Her visual acuity was only mildly affected. Clinical examination showed grade 1 conjunctival injection, grade 3 corneal and conjunctival epithelial staining, and decreased tear film break-up time (less than three seconds) in each eye.
• Management. We initiated topical anti-inflammatory therapy q.i.d. in each eye with Lotemax (loteprednol 0.5%, Bausch & Lomb) and nonpreserved artificial tears q3h in each eye. At the four-week follow-up visit, the patient’s symptoms were markedly improved, as were the ocular surface signs. We continued Lotemax b.i.d. for four more weeks and added Restasis (cyclosporine, Allergan) b.i.d. in each eye. During the next several weeks, we tapered the steroid and kept the patient on Restasis b.i.d. and artificial tears q.i.d. The patient’s signs and symptoms continued to improve. Twelve weeks after her initial visit, she successfully resumed contact lens wear.
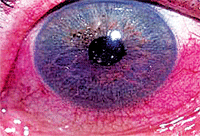 |
| Corneal and conjunctival surface dryness in a patient with secondary Sjögren’s syndrome (SS) can be treated with topical and systemic immunomodulatory therapy. |
In autoimmune disease, the immune system’s recognition apparatus breaks down, and the body begins to manufacture T cells and antibodies directed against its own cells and organs. Misguided T cells and autoantibodies contribute to the development of many diseases. For instance, T cells that attack the pancreas contribute to diabetes, while the autoantibody known as rheumatoid factor is common in people with rheumatoid arthritis (RA). People with systemic lupus erythematosus (SLE) have antibodies to many types of their own cells and cell components.4 Sjögren’s syndrome (SS) is an autoimmune disease characterized by progressive lymphocytic and plasma cell infiltration of the salivary and lacrimal glands. SS is the most common inflammatory condition that leads to tear-deficient dry eye syndrome.5
SS is categorized into two groups:5
• Primary SS, in which the patients do not fulfill criteria for another well-defined associated autoimmune disease.
• Secondary SS, in which symptoms and signs of dryness are associated with another well-defined autoimmune entity, such as SLE or RA.
| Autoimmunity and the Eye | |
| Condition
|
Ocular Manifestation(s)
|
| Ankylosing spondylitis
|
Uveitis |
| Antiphospholipid antibody syndrome
|
Ischemic optic neuropathy, retinal vascular occlusion |
| Behçet’s disease | Uveitis
|
| Giant cell arteritis
|
Optic neuropathy, amaurosis fugax, diplopia, retinal vascular occlusion |
| Graves’ disease | Proptosis/exophthalmos, keratitis, optic neuropathy |
| Multiple sclerosis | Optic neuritis, internuclear ophthalmoplegia, cranial nerve palsies |
| Myasthenia gravis
|
Diplopia, ptosis |
| Polyarteritis nodosa | Episcleritis/scleritis, optic neuropathy |
| Reiter’s syndrome | Conjunctivitis, uveitis, keratitis |
| Rheumatoid
arthritis
|
Keratoconjunctivitis sicca, scleritis/episcleritis, macular edema |
| Sarcoidosis | Uveitis, conjunctival nodules, cranial nerve palsies, optic neuropathy |
| Sjögren’s syndrome
|
Keratoconjunctivitis sicca |
| Systemic lupus erythematosus
|
Keratoconjunctivitis sicca, conjunctivitis, uveitis, episcleritis/scleritis, retinal hemorrhages, retinal vasculitis, optic neuropathy |
| Wegener’s granulomatosis
|
Proptosis/exophthalmos, orbital cellulitis, uveitis, corneal ulcer, optic neuropathy |
Ocular Surface Inflammation
Although the pathology of dry eye is multifactorial, researchers now think it occurs due to inflammation of the lacrimal gland and ocular surface when systemic androgen levels fall below a point needed to maintain an optimal environment.6 Inflammation may initially occur from the activation of T cells migrating through the lacrimal gland. Pro-inflammatory cytokines (interleukin 1-beta, interleukin-2, interferon and tumor necrosis factor-alpha) secreted by the activated lymphocytes may cause a disruption or inhibition of the nerve cell signal to the lacrimal gland in patients with autoimmune and non-autoimmune dry eye syndrome.2,3
Topical cyclosporine prevents the production of these pro-inflammatory cytokines by binding to a specific cytosolic protein called cyclophilin. The cyclosporine-cyclophilin complex blocks early T cell gene expression, which modulates unwanted immune-mediated inflammation.2,3,6
In addition to immunomodulation with topical cyclosporine, topical corticosteroids, such as prednisolone and loteprednol, have a beneficial effect both on the subjective symptoms and objective clinical measures of moderate-to-severe dry eye patients. These effects are associated with the reduction of inflammatory biomarkers of conjunctival epithelial cells.7 Corticosteroids inhibit arachidonic acid release from phospholipids, inhibit the transcription and action of cytokines, and limit B and T cell activity. They are used in inflammatory diseases of a noninfectious cause.8 Treatment with immunomodulatory agents results in resolution of acute inflammatory assault on ocular tissues. In ocular surface inflammatory disease, immunomodulatory therapy may lead to improved tear production and improvement of keratoconjunctivitis sicca.
Systemic immunosuppressive agents (such as methotrexate, prednisone, cyclophosphamide or cyclosporine) may also be required in the treatment of recalcitrant primary and secondary ocular inflammation caused by systemic autoimmune conditions.
Drs. Pelino and Pizzimenti have no financial interest in any of the products mentioned.
1. Niederkorn JY. Role of NKT cells in anterior chamber-associated immune deviation. Exp Rev Clin Immunol. 2009 Mar;5(2):137-44.
2. Kunert KS, Tisdale AS, Stern ME, et al. Analysis of topical cyclosporine treatment of patients with dry eye syndrome: Effect on conjunctival lymphocytes. Arch Ophthalmol. 2000 Nov;118(11):1489-96.
3. Stern ME, Beuerman RW, Fox RI, et al. The pathology of dry eye: the interaction between the ocular surface and lacrimal glands. Cornea. 1998 Nov;17(6):584-9.
4. Roitt I, Brostoff J, Male D. Immunology. 2nd ed. St. Louis: CV Mosby;1989.
5. Fox RI, Kang HI. Pathogenesis of Sjögren’s syndrome. Rheum Dis Clin North Am. 1992 Aug;18(3):517-38.
6. Pflugfelder SC. Antiinflammatory therapy for dry eye. Am J Ophthalmol. 2004 Feb;137(2):337-42.
7. Avunduk AM, Avunduk MC, Varnell ED, Kaufman HE. The comparison of efficacies of topical corticosteroids and nonsteroidal anti-inflammatory drops on dry eye patients: a clinical and immunocytochemical study. Am J Ophthalmol. 2003 Oct;136(4):593-602.
8. Janigian RH Jr, Young D. Uveitis, Evaluation and Treatment. eMedicine from WebMD website. Available at: http://emedicine.medscape.com/article/1209123-overview (accessed August 18, 2009).

