 A 42-year-old white female presented with complaints of blurred vision in both eyes at near. She also noted that her distance vision became blurrier recently. She reported no previous problems with her eyes and has never worn glasses. Her medical history was significant for controlled hypertension as well as a tumor in her right ear that was removed approximately four years earlier.
A 42-year-old white female presented with complaints of blurred vision in both eyes at near. She also noted that her distance vision became blurrier recently. She reported no previous problems with her eyes and has never worn glasses. Her medical history was significant for controlled hypertension as well as a tumor in her right ear that was removed approximately four years earlier.
Her uncorrected visual acuity measured 20/25 O.U.; with minimal hyperopic correction, she improved to 20/20 O.U. At near, however, she demonstrated J2 O.U. (with a correction of +1.25D, she improved to J1+).
Confrontation visual fields were full to careful finger counting O.U. Extraocular motility testing was normal. Her pupils were equally round and reactive to light, with no afferent pupillary defect. The anterior segment examination was unremarkable. Her intraocular pressure measured 19mm Hg O.U. On dilated fundus exam, she demonstrated a moderate-sized cup with good rim coloration and perfusion O.U. We documented obvious fundus changes adjacent to the macula in her right eye as well as definite retinal thickening (figure 1). The periphery was unremarkable. The fundus examination of her left eye was completely normal (figure 2). We also ordered a spectral domain optical coherence tomography of her right eye (figure 3).
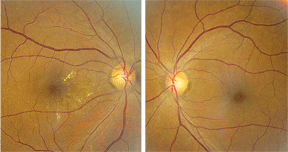 |
| 1, 2. Fundus images of our patient (O.D. left, O.S. right). Note the changes seen near the macula in her right eye.
|
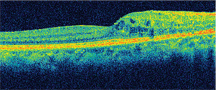 |
| 3. What does this SD-OCT reveal about the patient’s macula O.D.? |
Take the Retina Quiz
1. What do the fundus changes in her right eye represent?
a. Exudate.
b. Cotton wool spots.
c. Fibrin.
d. Dehemoglobinized blood.
2. What does the SD-OCT show?
a. Normal macula.
b. Serous detachment.
c. Macular schisis.
d. Cystoid macular edema (CME).
3. What is the likely diagnosis?
a. Non-proliferative diabetic retinopathy.
b. Type 1 macular telangiectasia.
c. Hypertensive retinopathy.
d. Radiation retinopathy.
4. How should we manage this patient?
a. Close observation.
b. Focal laser.
c. Intravitreal Kenalog (triamcinolone, Bristol-Myers Squibb).
d. Intravitreal Avastin (bevacizumab, Genentech).
For answers, see below.
Discussion
The macular changes seen in our patient represent radiation retinopathy. Upon further questioning, our patient stated that she had an auditory canal tumor removed from her right ear approximately four years earlier. Then, she received chemotherapy and underwent 10 sessions of external beam radiation treatment to her ear. Radiation retinopathy is an occlusive microangiopathy that develops as a result of ionizing radiation. The condition is often caused by exposure to radiation from a radioactive plaque or by external beam radiation treatment for ocular, orbital and intracranial tumors. It has also been reported to occur following radiation treatment for Graves’ ophthalmopathy.1
Radiation retinopathy is characterized by microaneurysms, capillary dropout and neovascularization. Retinopathy develops from endothelial cell loss and capillary closure within the retinal vessels as a form of collateral damage from the ionizing radiation treatment.
Additionally, macular edema is a common result of leaky capillaries. The degree of visual loss is dependent on the extent of vessel damage and non-perfusion. Clinically, radiation retinopathy can appear similar, if not identical, to hypertensive or diabetic retinopathy.
So, both a comprehensive patient history and a careful examination of the fellow eye are critical to making an accurate diagnosis. For example, our patient’s left eye is completely normal, which would be unusual in a case of hypertensive or diabetic retinopathy. Interestingly, radiation retinopathy has a delayed onset of months to years following radiation treatment. Typically, the condition progresses slowly, and its severity is dependent on the total dose of radiation, the daily fraction size, the fraction interval, how close in proximity the retina is to where the radiation was directed, and how much radiation exposure the retina and ocular structures received.
Typically, patients on radiation therapy receive 2 Gy to 3 Gy per day, with a total course ranging from 35 Gy to 72 Gy. The usual threshold dose for retinal damage is approximately 30 Gy to 35 Gy, but the lowest reported dose of radiation that caused radiation retinopathy is 11 Gy.1 Photoreceptors are more resistant to radiation than inner retinal layers and retinal vascular cells. In addition to radiation retinopathy, radiation therapy can cause ischemic retinopathy, vessel closure and severe dry eye.
Laser treatment is indicated for radiation retinopathy that results in neovascularization from either proliferative disease or from macular edema. Anti-vascular endothelial growth factor (VEGF) drugs, such as Avastin (bevacizumab, Genentech), have also increased as a standard treatment for radiation retinopathy.2
Our patient demonstrated clear retinal thickening in close proximity to the macula of her right eye. In this case, we considered this thickening to be indicative of macular edema. And indeed, SD-OCT confirmed the existence of CME. Given that our patient saw 20/20 O.D. and remained asymptomatic, we elected for close management without any treatment for the time being. However, if her CME progresses or she begins to suffer any visual loss, we will discuss further treatment options, including Avastin injection.
1. Murray TG, Christmas N. 53-year-old female complaining of “seeing blood” O.U. for four weeks. Digital J Ophthalmol. 1996;2(4):1-7.
2. Gupta A, Muecke JS. Treatment of radiation maculopathy with intravitreal injection of bevacizumab (Avastin). Retina. 2008 Jul-Aug;28(7):964-8.
Retina Quiz Answers: 1) a; 2) d; 3) d; 4) a.

