History
A 47-year-old black female presented with a chief complaint of blurry vision in her right eye. She explained that her vision had been poor since she underwent retinal reattachment surgery secondary to advanced proliferative diabetic retinopathy (PDR) OS six months earlier.
Her ocular history was remarkable for PDR OU, which was treated with panretinal photocoagulation (PRP) and vascular endotheilial growth factor (VEGF) inhibitor injections; clinically significant macular edema OU, which was treated with focal laser and VEGF therapy; and tractional retinal detachment OS, which was repaired by a retina specialist six months prior.
Her systemic history was remarkable for hypertension and type 1 diabetes mellitus, which were properly controlled with valsartan/hydrochlorothiazide, metformin, glipizide and insulin.
She reported no known allergies of any kind.
Diagnostic Data
Her best-corrected visual acuity measured 20/50 OD and 20/100 OS at distance and near. Her external examination uncovered an afferent pupillary defect OS, with a decompensated esophoria secondary to unsustainable fixation. She was pseudophakic OS, with posterior capsular opacification.
|
|
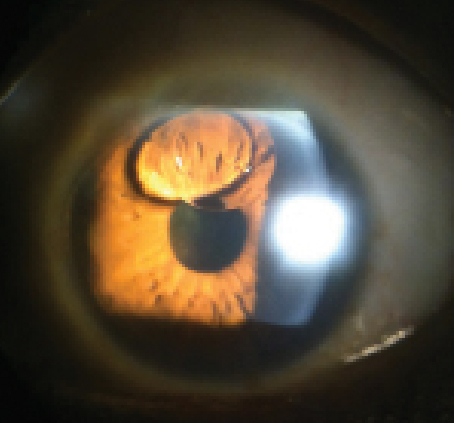
| This patient with a history of proliferative diabetic retinopathy reported poor vision in her left eye following retinal reattachment surgery. What is the correct diagnosis? |
|
Intraocular pressure measured 15mm Hg OU. Dilated fundus evaluation revealed areas of dense PRP OU, evidence of focal laser to both maculae, and an attached and flat retina OS with no new neovascular fronds or retinal breaks.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What’s the likely prognosis?
Discussion
Further evaluation included photodocumentation, as well as additional refraction and laser interferometry to determine the patient’s best visual potential. We also placed a call to the retinologist who performed the detachment surgery earlier in the year.
The diagnosis in this case is a silicone oil bubble in the anterior chamber OS. Surgical silicone oil, also known as dimethicone, is a popular type of polydimethylsiloxane that features low surface tension, good shear resistance and excellent thermal stability.1 The agent is available in several different viscosities.1 Typically, 1,000cs or 5,000cs fluid is used as an intravitreal tamponading agent in surgery for rhegmatogenous retinal detachment cases that are complicated by proliferative vitreoretinopathy.1-3
Although silicone oil is important in the treatment of complex forms of retinal detachment, controversy still surrounds the issue of selecting the proper viscosity for clinical use.1-3 In complicated retinal detachment surgery, the use of 5,000cs silicone oil may be associated with poorer anatomic and visual outcomes compared to those achieved using 1,000cs silicone oil.1 Other studies have shown no differences, rendering the viscosity and choice of the tamponade agent an individualized decision for each patient and his or her circumstances.2
Several reports have concluded that the agent can migrate into the retina and the optic nerve, potentially causing myelinated optic nerve fiber loss.3 Thus, researchers recommend exercising caution when using silicone oil in eyes with complicated retinal detachments that have good visual potential.3
The use of silicone oil for the treatment of complicated retinal detachment was first described in 1962.4 Combined with vitreoretinal surgery, silicone oil injection has become a standard technique to improve the prognosis of complex retinal detachment associated with proliferative vitreoretinopathy, giant retinal tears, proliferative diabetic retinopathy or ocular trauma.1-4
In some studies, eyes treated with silicone oil were more likely to be successfully reattached than those treated with sulphur hexafluoride gas.4 More specifically, those receiving silicone oil injection achieved a better visual outcome and fewer postoperative complications.4
However, silicone oil has the potential to cause several long-term complications, including cataract formation, glaucoma and keratopathy. To avoid these potential difficulties, retinologists generally recommend silicone oil removal as soon as a stable retinal solution is achieved.4 Unfortunately, the removal procedure itself increases the patient’s risk of other ocular complications––namely retinal redetachment secondary to reproliferation of epiretinal membranes and additional retinal traction.4
One study proposed four different mechanisms that could cause glaucoma following silicone oil injection:5
• Overfill of the posterior chamber, leading to total anterior chamber fill and mechanical obstruction of aqueous outflow.
• Silicone oil pupillary block.
• Denaturation of the silicone oil into microdroplets, which become deposited in the trabecular meshwork and cause secondary open-angle glaucoma.
• Secondary inflammation, which may exacerbate pre-existing glaucoma.
Optic neuropathy associated with silicone oil injection was initially attributed to its ability to penetrate the optic nerve via retrolaminar migration; intracranial migration via this mechanism is very uncommon. Migration into the optic nerve has not been formally demonstrated in human post-mortem studies.6 Other factors, such as glaucomatous damage to the disc region and active transport mechanisms, are thought be involved in the development of silicone oil-associated optic neuropathy.6
Cataract formation is the most common complication following silicone oil injection. The primary causative factor for cataract formation is oxidative stress, however; mechanical considerations, such as direct contact between the oil and the lens also can lead to desiccation cataract.7
Corneal endothelial decompensation is another frequent complication when silicone oil is used for the treatment of proliferative vitreoretinopathy.8 Corneal edema, corneal hypesthesia, endothelial opacification, band keratopathy and peripheral corneal vascularization all have been documented.8
Multiple studies examining the effect of 1,000cs and 5,000cs on corneal endothelial cells revealed that these agents have may induce endothelial cell proliferation inhibition. Here, silicone oil cytotoxicity actually appears to be cultivated in human endothelial cells.9 Therefore, minimizing the forward migration of silicone oil into the anterior chamber is a fundamental goal so that keratopathy can be avoided.4,9
We referred our patient for cataract surgery OD, because refraction failed to elevate visual acuity to an acceptable level. Because laser interferometry indicated that the visual loss in her left eye was the result of diabetic retinopathy and several surgical procedures, no YAG capsulotomy was arranged. Following a consultation with retinology, we determined that no additional intervention was warranted because the silicone bubble was not inducing corneal decompensation or increased intraocular pressure.
We will monitor her at four- to six-month intervals to rule out neovascularization of the iris, disc and elsewhere, and to insure the bubble causes no anterior segment or glaucomatous complications.
Thanks to Peter J. Perno, BS, a fourth-year student at Salus University in Elkins Park, Pa., for his contributions to this case.
1. Soheilian M, Mazareei M, Mohammadpour M, Rahmani B. Comparison of silicone oil removal with various viscosities after complex retinal detachment surgery.
BMC Ophthalmol. 2006 May 31;6:21.
2. Schwartz SG, Flynn HW Jr, Lee WH, Wang X. Tamponade in surgery for retinal detachment associated with proliferative vitreoretinopathy.
Cochrane Database Syst Rev.
2014 Feb 14;2:CD006126.
3. la Cour M1, Lux A, Heegaard S. Visual loss under silicone oil.
Klin Monbl Augenheilkd.
2010 Mar;227(3):181-4.
4. Falkner CI, Binder S, Kruger A. Outcome after silicone oil removal. Br J Ophthalmol. 2001 Nov;85(11):1324-7.
5. Ichhpujani P, Jindal A, Katz L. Silicone oil induced glaucoma: a review. Graefes Arch Clin Exp Ophthalmol. 2009 Dec;247(12):1585-93.
6. Grzybowski A, Pieczynski J, Ascaso FJ. Neuronal complications of intravitreal silicone oil: an updated review. Acta Ophthalmol. 2014 May;92(3):201-4.
7. Milazzo S. Pathogenesis of cataract after vitrectomy. J Fr Ophtalmol. 2014 Mar;37(3):243-4.
8.
Foulks GN
,
Hatchell DL
,
Proia AD
,
Klintworth GK
. Histopathology of silicone oil keratopathy in humans.
Cornea.
1991 Jan;10(1):29-37.
9.
Yang CS
,
Chen KH
,
Hsu WM
,
Li YS
. Cytotoxicity of silicone oil on cultivated human corneal endothelium.
Eye (Lond).
2008 Feb;22(2):282-8.

