 A 79-year-old white female presented with complaints of decreased visual acuity in her right eye. The patient's ocular history was significant for open-angle glaucoma.
A 79-year-old white female presented with complaints of decreased visual acuity in her right eye. The patient's ocular history was significant for open-angle glaucoma.
She initially converted to glaucoma in 2003 because of a consistent rise in untreated IOP into the upper 20s as well as subtle changes to her neuroretinal rims in both eyes. At that time, we stabilized her IOP with 1 gtt Lumigan (bimatoprost 0.03%, Allergan) O.U. h.s., which she tolerated well.
In addition to Lumigan, her current ophthalmic medications included Actonel (risedronate sodium, Proctor & Gamble Pharmaceuticals) Lipitor (atorvastatin, Pfizer) and Synthroid (levothyroxine sodium, Abbott Laboratories). Neither her ocular nor her systemic medications had been changed in the past four years.
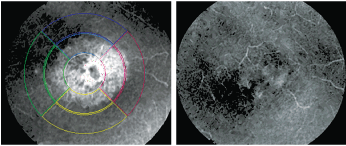
Our patient's postoperative HRT-3 scan clearly showed an increase in edema in the central macula O.D. Note the cystic appearance of the central foveal avascular zone (left). After six weeks of treatment with Pred Forte and Nevanac, her visual acuity returned to 20/25-. Note the significant reduction of CME in the central macula.
Diagnostic Data
Preoperatively, her best-corrected visual acuity measured 20/60 O.D. and 20/30- O.S. through myopic astigmatic correction. Her pupils were equally round and reactive to light and accommodation, with no afferent pupillary defect. Her extraocular motilities were full in all positions of gaze.
Her anterior segments were essentially unremarkable, except for mild corneal arcus O.U. As our patients cataracts progressed, her anterior chamber angles narrowed. Her angles, as estimated by Van Hericks method, were grade 2+ open O.U., which was confirmed on gonioscopy.
There was a mild amount of trabecular pigmentation O.U., with no angle abnormalities. Pachymetry readings were 553m O.D. and 564m O.S. While medicated with Lumigan, her intraocular pressure measured an average of 14mm Hg O.D. and 15mm Hg O.S.
Through dilated pupils, her crystalline lenses were characterized by grade 3 nuclear sclerosis O.D. and grade 2 nuclear sclerosis O.S. Additionally, she exhibited mild posterior sub-capsular opacification O.D. off the visual axis. She also had bilateral posterior vitreous detachments.
Her optic nerves were characterized by 0.50 x 0.65 cupping O.D. and 0.50 x 0.60 cupping O.S. The optic nerves were of normal size, and the cups were slightly displaced temporally. The inferior temporal neuroretinal rims were marginally thinned in both eyes.
Heidelberg Retina Tomograph-3 (HRT-3, Heidelberg Engineering) imaging and stereophotography confirmed the clinical observations of the optic nerves and neuroretinal rims. Both maculae were characterized by fine retinal pigment epithelium granulation that was
consistent with her age. The peripheral retinal examinations were normal in both eyes.
Given the progressively decreasing visual acuity in her right eye and its interference with her quality of life, we scheduled her for cataract surgery.
Discussion
Given the mechanism of action of prostaglandin analogues (PGAs) and their tendency to incite anterior uveitis, some clinicians discontinue PGAs prior to cataract surgery and substitute another glaucoma medication during the perioperative period. Several early studies implicated latanoprost with a higher incidence of cystoid macular edema in uncomplicated phacoemulsification.1-3
Yet, other studies have shown that prostaglandin use during the cataract perioperative period does not play a role in increasing the likelihood of postoperative uveitis and CME.4,5 And, in accordance with these studies, our protocol has changed--we no longer discontinue PGAs prior to cataract surgery unless the patient already demonstrates a problem associated with their use, such as hyperemia or pre-existing anterior uveitis.
Our patient underwent uncomplicated, clear corneal cataract surgery in her right eye in the fall of 2008. We medicated her with Vigamox (moxifloxacin, Alcon) q.i.d., Xibrom (bromfenac, ISTA Pharmaceuticals) b.i.d. and Econopred Plus (prednisolone acetate, Alcon) q.i.d. We also continued her on Lumigan.
At the one-week postoperative follow-up, her uncorrected visual acuity measured 20/25- O.D. The anterior chamber was characterized by trace cell and no flare. The IOL was clear and centered in the capsular bag, and the posterior capsule was intact. The wound was tight with a negative Siedel sign, and the overlying epithelium was intact. Her IOP measured 12mm Hg O.D. and 14mm Hg O.S. Her retinal and optic nerves remained unchanged after surgery.
At that visit, we told her to continue the Xibrom b.i.d. until the bottle was empty; discontinue the Vigamox; and taper the Econopred Plus to q.i.d. for one week, t.i.d. for one week, b.i.d. for one week and q.d. for one week. We scheduled her for a second follow-up in one month.
Three weeks later, the patient presented with complaints of decreased visual acuity in her right eye. She reported no pain, photophobia or photopsia. At this visit, her visual acuity had decreased to 20/50- O.D. Her anterior chamber was characterized by trace cell and no flare, and her IOP measured 13mm Hg O.D. The IOL was centered and the capsule was intact.
On fundoscopic examination, she demonstrated retinal findings consistent with CME.
CME is most commonly seen following cataract surgery, but it is also associated with diabetic retinopathy, collagen vascular disease, aphakia in conjunction with epinephrine agents, and after retinal detachment repair. CME is likely precipitated by the production of prostaglandins, which is induced by surgical trauma to the anterior segment, particularly the iris. CME is more commonly found after intracapsular cataract extractions than extracapsular procedures.
Treatment of CME is straightforward and aims to reduce the underlying inflammation. Treatment may include oral and/or topical non-steroidal anti-inflammatory drugs and topical steroids. More chronic cases may respond to more aggressive therapies, such as a sub-Tenons injection of steroids.
Given the classic findings of CME, I asked our patient to discontinue the Econopred Plus and begin Pred Forte (prednisolone acetate, Allergan) q4h while awake and Nevanac (nepafenac, Alcon) q.i.d. We decided to make this switch because Pred Forte not only has been shown to mix better after shaking than Econopred, but also the acetate form of prednisolone better penetrates the eye than the phosphate form found in other prednisolone preparations.
During the next six weeks, our patient's macular edema decreased significantly as we slowly tapered both the steroids and NSAIDs after achieving initial improvement in the CME. Her uncorrected visual acuity returned to 20/25- O.D., and she has experienced no recurrence of CME to date.
Still, the question remained: What was the fundamental cause of our patients CME? Was this patient's CME related to glaucoma? Was it related to continued PGA use throughout the perioperative period? In hindsight, the answer became clear.
In addition to our patient, two others who underwent uncomplicated cataract surgery at the hands of the same surgeon presented with CME within a month after surgery. This increased incidence of CME was quite rare compared with previous years. The probable cause: A change in the postoperative regimen. Previously, we prescribed Pred Forte as a post-op anti-inflammatory steroid drop. In these cases, however, we treated the patients with Econopred Plus. Otherwise, all intraoperative techniques remained unchanged.
Nevertheless, all cases of CME were resolved with aggressive anti-inflammatory therapy. Rest assured, though, that the literature supports concurrent use of PGAs in your glaucoma patients undergoing cataract surgery.
1. Yeh PC, Ramanathan S. Latanoprost and clinically significant cystoid macular edema after uneventful phacoemulsification with intraocular lens implantation. J Cataract Refract Surg. 2002 Oct;28(10):1814-8.
2. Altintas O, Yksel N, Karabas VL, Demirci G. Cystoid macular edema associated with latanoprost after uncomplicated cataract surgery. Eur J Ophthalmol. 2005 Jan-Feb;15(1):158-61
3. Dhingra N, Morgan JE. Pseudophakic cystoid macular oedema: 30 months after latanoprost challenge. Eye. 2007 Feb;21(2):269-71.
4. Wand M, Shields BM. Cystoid macular edema in the era of ocular hypotensive lipids. Am J Ophthalmol. 2002 Mar;133(3):393-7.
5. Law SK. Clinical cystoid macular edema after cataract surgery. J Glaucoma. 2009 Jun 12. [Epub ahead of print]

